Good is your edge, and we always find it — no matter the assignment.
Our clients’ common thread? Purpose. Whether it’s CPG, health & well-being, outdoor & environment, or a combo of all three.

CU Division of Continuing Education
We built a multi-year campaign that repositions CE within the lived experience of credit-seeking students, driven by key audience and brand equity insights.
CU Division of Continuing Education

Protect Our Winters
We crafted web experiences that make the most of every scroll to encourage more people to protect the outdoor places they love from climate change.
Protect Our Winters

East Bay Community Foundation
We reinvented the foundation's identity to boldly and confidently renew their legitimacy with a look and feel as inclusive and diverse as the audiences they serve.
East Bay Community Foundation
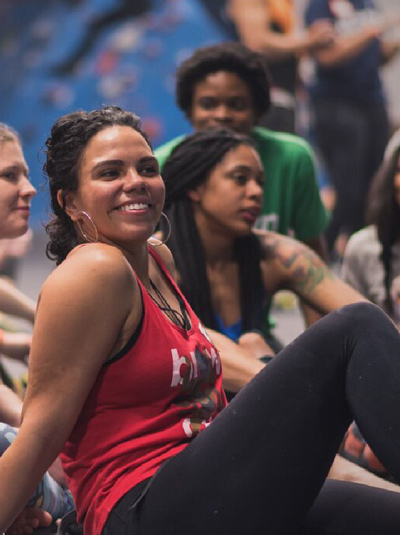
Movement Gyms
We built a fiercely inclusive new brand for the nation’s largest community of climbing, yoga, and fitness gyms.
Movement Gyms

jack & annie's
We built deliciously enticing digital campaigns to encourage a planet- and palate-friendlier way to go meatless.
jack & annie's

Appalachian Mountain Club
We developed a scroll-stopping digital campaign that invites a new generation of nature lovers to get outside and Do Something Indescribable.
Appalachian Mountain Club
"*" indicates required fields